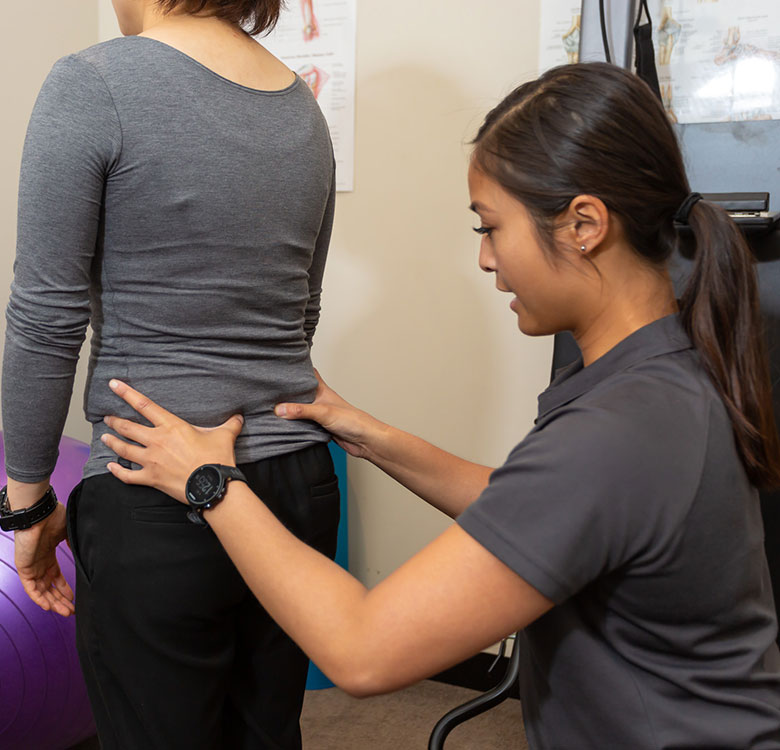
Commonly called “herniated disc” or “ruptured disc” (or misleadingly called “slipped disc”), a disc prolapse is one of the common conditions we treat. The spinal column is made up of a number of bones called vertebrae. Between these vertebrae are discs which prevent the bones from rubbing against each other during movement and act as shock absorbers during impact. In the lumbar spine (lower back), the discs are composed of a fibrous outer layer and a gel-like inner layer. When the outer layer becomes worn through overuse or injury, the inner layer can leak or “prolapse” out of the disc and cause pain.
Sometimes all it takes is a sudden, forceful movement (such as bending or lifting) to put too much strain on an already weakened disc and cause severe pain. If the prolapsed substance touches a nerve, pain, weakness and reduced sensation can be felt along the nerve, usually down the buttock or leg. This is known as sciatica. Staying active during the acute stages is preferred over bed rest, as long as the activity does not aggravate the pain. This is why an early visit to your physiotherapist is critical in repairing the disc and relieving pain.
Your Physio will perform a thorough assessment which would include various neurological, orthopaedic and other tests. We will then apply pain-relieving modalities which may include ultrasound, ice and heat packs. The next step will be joint mobilisation and exercises to reduce stiffness, restore mobility and promote healing of the damaged disc. Specific stretching and strengthening exercises to increase mobility and muscle strength and prevent further deterioration of the disc will follow.
Once healing begins to take place, we will tailor an exercise program that suits your needs and lifestyle. Core strengthening exercises that tighten the abdominal wall are usually recommended to promote good posture and restore normal function. Education in proper body mechanics such as lifting, bending, work habits etc. is vital in preventing a recurrence of the injury.
Please give us a call on (03) 9873 3333 or email us if you would like to book an appointment or for further information.